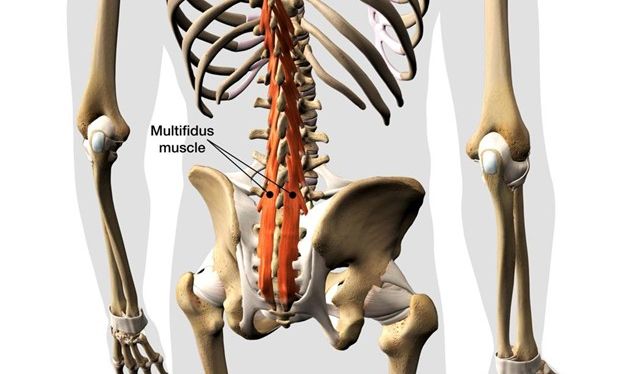
Multifidus Dysfunction: A Hidden Cause of Chronic Low Back Pain
What Is the Multifidus Muscle?
The multifidus is a deep muscle that runs along your spine. It connects one spinal bone (vertebra) to the next.
Unlike larger muscles that move your body, the multifidus is a stabilizer. Its job is to control small, precise movements between each spinal segment.
It helps:
• Keep your spine properly aligned • Control small movements between vertebrae • Protect discs and joints from too much stress • Support good posture • Keep your spine stable during bending, lifting, and twisting
In a healthy spine, the multifidus turns on before you move. It creates a stable base so your body can move safely.
What Is Multifidus Dysfunction?
Multifidus dysfunction happens when this deep stabilizing muscle shuts down, becomes weak, or starts to shrink.
This often happens after:
• A low back injury • A disc problem like a herniation or degeneration • Repeated episodes of back pain • Back surgery • Long periods of inactivity
After an injury, the body can actually shut the multifidus off at the segmental level through a neurological reflex called athrogenic muscle inhibition.
Arthrogenic muscle inhibition (AMI) is a reflex response where the nervous system reduces the signals to the muscles surrounding an injured joint, leading to a decrease in muscle activity. This inhibition can result in muscle atrophy and fatty replacement of the multifidus muscle, which is crucial for stabilizing the spinal vertebra. The process is often exacerbated by persistent pain signals from the back, leading to a cycle of pain which leads to inhibition, inhibition leads to weakness, and weakness leads to more stress on the spine and more pain.
A Simple Way to Understand It
Think of it like a circuit breaker in your house.
If there is a surge or a problem, the breaker trips to prevent damage. Power gets shut off, not because the system is broken, but to protect it.
The same thing happens in your spine.
When a disc, joint, or ligament is irritated, your nervous system senses a problem and “trips the breaker.” It reduces the signal going to the stabilizing muscles, including the multifidus.
So even if you try to contract the muscle, the signal is being limited.
The muscle is just not fully turning on; the system has to be reset.
And just like a circuit breaker, fixing the original issue does not always turn things back on automatically.
Why Does This Happen in the Spine?
When structures like discs, facet joints, ligaments, or joint capsules are irritated, they send signals to the brain and spinal cord.
The nervous system reads this as a threat and responds by reducing activation to nearby stabilizing muscles.
This involves several types of receptors:
• Mechanoreceptors (sense movement and position) • Nociceptors (sense pain and inflammation) • Joint capsule receptors
These signals travel through the spinal cord to the brain, which then reduces the activity of the motor nerves that control stabilizing muscles.
This happens at both the spinal cord level and the brain level.
The result:
• Decreased muscle activation • Poor spinal stability • Ongoing weakness even after pain improves
Even when pain gets better, the muscle often does not turn back on by itself.
Why the Multifidus Is So Affected
The multifidus is especially vulnerable because it controls small, precise movements in the spine.
After a lumbar injury:
• The muscle can weaken within days • It can start to shrink quickly • It often shrinks more on the injured side • Fat can replace healthy muscle if the problem continues
And again, this does not automatically recover when pain improves.
Why This Matters
If the multifidus is not working:
• The spine loses fine motor control • Larger muscles try to take over • Stress increases on discs and joints • Pain is more likely to come back
You can still move, but your spine loses its internal support system.
This explains why many patients feel better for a while, then the pain returns.
Over time, this leads to:
• Progressive muscle loss (atrophy) • Delayed muscle activation • Loss of segmental control • Fat replacing muscle
Why Multifidus Dysfunction Matters
Segmental Instability
Without deep stability, small parts of the spine move too much. Larger muscles try to compensate, but they are not designed for this job.
Increased Disc and Joint Stress
Too much small movement increases stress on discs and joints, which can speed up degeneration.
Repeating Pain Cycles
Instability leads to irritation → inflammation → muscle guarding → more shutdown → worsening instability.
False Strength
Some patients look strong but lack deep stabilizer function. Many exercise programs miss this.
What Imaging Often Shows
In chronic low back pain, imaging may show:
• Multifidus muscle loss • Side-to-side differences • Fatty replacement of muscle • Ongoing atrophy even after symptoms improve
This explains why patients:
• Improve temporarily • Feel better with basic exercise • Relapse when returning to normal activity
Because the stabilizing system was never fully restored.
Why Pelvic Stabilization Is Critical
One of the most overlooked parts of spinal rehab is pelvic control.
If the pelvis is not stabilized:
• Larger muscles take over • The spine moves without control • The multifidus stays underactive • Exercises become less effective
The pelvis is the foundation of the lower spine. If it moves too much, patients can “cheat” exercises using larger muscles.
Proper pelvic stabilization:
• Locks the hips in place • Removes momentum • Prevents compensation • Forces deep spinal muscles to work • Allows true isolation of the multifidus
Without stabilizing the pelvis, it is very difficult to target this muscle.
Why Standard Core Exercises Often Fail
Most programs focus on:
• Planks • Crunches • Sit-ups • General strengthening
These mainly work larger muscles like:
• Abdominals • Obliques • Erector spinae • Hip flexors
These help with fitness, but they do not fix deep stabilizers.
As a result, patients often:
• Plateau • Have recurring pain • Develop poor movement patterns • Feel stronger but are still unstable
The Role of MedX in Treating Multifidus Dysfunction
1. Accurate Measurement
MedX spinal strength testing:
• Measures lumbar strength objectively • Identifies specific weak areas • Shows how much function is lost • Tracks progress over time
This removes guesswork and targets the real problem.
2. Pelvic Stabilization
The key feature of MedX is pelvic stabilization.
The MedX machine:
• Locks the pelvis and hips in place • Prevents compensation from glutes, hips and hamstrings • Eliminates momentum • Forces deep spinal muscles to work • Maximizes multifidus activation
Without this, most “back exercises” become hip and leg exercises.
3. Targeted Strengthening
With proper isolation:
• Deep stabilizers are safely strengthened • Muscle control improves • Segmental stability returns • Muscle loss can reverse • The spine can handle more load
4. Structured, Measurable Progress
MedX programs use:
• Controlled movement • Gradual resistance • Regular re-testing • Data-driven progression
This leads to predictable, measurable outcomes.
What Happens If This Is Not Treated
If the multifidus stays weak:
• Chronic back pain continues • Disc problems are more likely to return • Degeneration in the discs and facet joints speeds up • Activity tolerance declines • Fear of movement increases
Patients often get stuck in a cycle of temporary relief followed by flare-ups.
What Happens When Stability Is Restored
When the multifidus starts working again:
• The spine regains control • Disc stress decreases • Movement improves • Flare-ups happen less often • Strength and function increase • Confidence returns
Spinal stability is the foundation for long-term recovery!
In conclusion
Chronic low back pain is often not just a disc problem or a muscle strain.
It is often a failure of the spine’s deep stabilizing system.
Multifidus dysfunction cannot be fixed with general exercise alone. It requires:
• Objective strength testing • Proper pelvic stabilization • True muscle isolation • Targeted, progressive rehab
MedX spinal testing and rehabilitation allow us to identify and correct the real problem that many treatments miss.
When you restore stability, you are not just treating symptoms. You are fixing the root cause and building a stronger, more resilient spine.